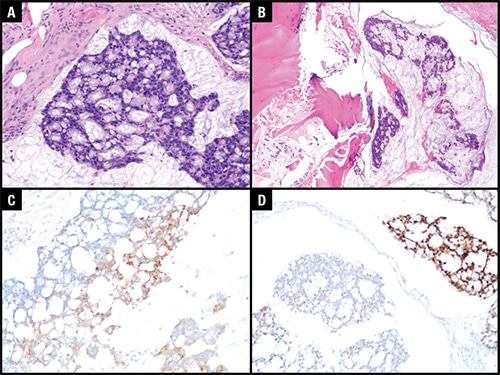
April 2020—IMpassion130 was the first phase three trial to demonstrate a clinical benefit of cancer immunotherapy in patients with PD-L1-positive metastatic triple-negative breast cancer, and based on the data, atezolizumab plus nab-paclitaxel is approved for this indication. In the trial, the Ventana SP142 PD-L1 assay with a one percent or greater cutoff was used to evaluate PD-L1 expression in immune cells. But questions remained about how to best identify patients who could benefit from the drug combination, Hope S. Rugo, MD, professor of medicine and director of breast oncology and clinical trials education at the University of California San Francisco Comprehensive Cancer Center, said in a CAP TODAY webinar last November.
Read More »Study: Combined DNA-RNA testing improves detection of MET mutations
March 2020—DNA and RNA sequencing, when used together, can improve detection of MET exon 14 skipping mutations in lung adenocarcinoma compared with DNA testing alone, according to a study reported last November at the Association for Molecular Pathology meeting. While RNA analysis can play an important complementary role to DNA analysis in detecting the mutation, it can also pick up false-positives if RNA analysis data are not adjusted properly, David Manthei, MD, PhD, a fellow in the University of Michigan Department of Pathology, explained in presenting the data. In the study, 482 cases of non-small cell lung cancer were sequenced using the Oncomine Focus Assay, a Thermo Fisher Scientific next-generation sequencing assay that conducts DNA and RNA analysis in a single workflow.
Read More »Technological advances enhance liquid biopsy’s clout
February 2020—New microfluidic and nanotechnologies could take liquid biopsy to the next level as a tool to gauge cancer progression and treatment response.
Read More »Carcinoma of unknown primary case reviewed in tumor board session
January 2020—A molecular oncology tumor board session at CAP19 explored a case of cancer of unknown primary, presented by medical oncologist Alexander Drilon, MD, research director of early drug development at Memorial Sloan Kettering Cancer Center, and Rondell P. Graham, MBBS, head of GI/liver pathology at Mayo Clinic Rochester.
Read More »Mate pair sequencing yields rich new data
November 2019—The LUVOIR telescope proposed this year by NASA, when it is launched into orbit, will outperform the Hubble Telescope 40-fold in ability to detect and visualize deep space objects in detail. But while dazzling in concept, the LUVOIR is still in development. Interestingly, at the genomic level, a similarly impressive advance in detection called mate pair sequencing has already progressed from research to clinical use in diagnosing cancer. With mate pair sequencing, a novel next-generation sequencing technique, Mayo Clinic is advancing the laboratory’s current capabilities for visualizing genetic rearrangements, thus increasing the diagnostic yield of testing for a variety of neoplasms.
Read More »NTRK fusion testing: ups, downs of four methods
November 2019—With two inhibitors approved by the FDA for the treatment of NTRK-fusion-positive solid tumors, the next step is to determine whom to test and how. If the efficacy of the compounds—larotrectinib and entrectinib—were the only thing to consider in implementing a testing algorithm, knowing whom to test would be easy.
Read More »For GI cancer, a digital and molecular reset
October 2019—You may not be curling up next to the fire with a cup of hot chocolate to read your copy of the new Digestive System Tumours, part of the World Health Organization Classification of Tumours Series.
Read More »AMP case report: Use of MYD88 sequencing to confirm diagnosis of PIOL in a case with limited sample availability
October 2019—Primary intraocular lymphoma (PIOL) is a rare but aggressive B-cell malignancy usually considered as a subtype of primary central nervous system lymphoma. The most common form of PIOL is primary vitreoretinal lymphoma. PIOL is also known as the masquerade syndrome because it frequently mimics other ocular conditions such as chronic uveitis, which may be steroid-resistant. Its diagnosis is challenging and requires a high degree of suspicion. Here, we present a case of PIOL, the diagnosis of which was clinched based on the identification of a mutation in the myeloid differentiation factor 88 (MYD88) gene.
Read More »AMP case report: NGS of a rare metastatic bladder adenocarcinoma
September 2019—Primary bladder adenocarcinoma is a rare vesicle malignancy accounting for up to two percent of malignant neoplasms of the bladder.1 They occur in males more than females and are classically seen in the fifth or sixth decade of life.2 Histologically they are of enteric, mucinous, or mixed types. Morphologically, the enteric type appears identical to a colonic adenocarcinoma and the mucinous type appears as neoplastic cells floating in pools of extravasated mucin. The mixed type is a mixture of the morphologies of the enteric and mucinous types. Immunohistochemically, adenocarcinomas of the urinary bladder classically express CK20 and CDX2.
Read More »Path to importance of PD-L1 status in breast cancer
June 2019—New data support testing patients for their PD-L1 immune cell status when they are diagnosed with metastatic or unresectable locally advanced triple-negative breast cancer to determine if they might benefit from a checkpoint inhibitor.
Read More »Bladder cancer detection and surveillance: How urine cell-free DNA stacks up against cytology
June 2019—A high-throughput sequencing panel was found to be more than 90 percent sensitive in detecting urinary tumor DNA in early-stage bladder cancer and in post-treatment surveillance. The approach, reported in April in Cancer Discovery, overcomes some of the challenges urinary cell-free DNA analysis poses, said one of its developers, and is far more sensitive than cytology and cystoscopy.
Read More »Wading deeper into liquid biopsy
March 2019—The standard riff for talking about a promising new cancer test should be familiar to anyone within sneezing distance of a laboratory: There’s no one-size-fits-all assay. But if any test were to come close, it would be liquid biopsy. Are clinicians eager to use it? Check. Is it relatively simple to do (check) with fairly quick turnaround times (check)? Does it work for solid and hematological tumors? Check and check. Across multiple specimen types—serum, urine, vitreous fluid, cerebrospinal fluid, stool? Quite likely. Can it be used to characterize patients’ molecular profiles, monitor therapy, assess tumor evolution, identify resistance mechanisms, and detect early disease and minimal/measurable residual disease? Half a dozen checks. Even if liquid biopsy does fall short of a one-size-fits-all assay, it’s doing a reasonable impression of a Swiss Army knife (if not Sergeant Troy’s sword fantastic, for those of you who are Thomas Hardy fans).
Read More »AMP case report: FDA-approved DNA blood test for colorectal cancer prompts patient to undergo colonoscopy
March 2019—Colorectal cancer is the third most diagnosed cancer and the second highest cause of cancer mortality in men and women, and in 2016 it accounted for about nine percent of all diagnosed cancers in the United States. When CRC is detected at an early localized stage, the five-year survival rate is 90 percent. With progression to regional disease, five-year survival remains high, at 71 percent.
Read More »Apocrine breast cancer, ESR1 mutations at center of tumor board review
February 2019—Two breast cases—one of apocrine carcinoma and androgen receptor overexpression and another of metastatic ER-positive cancer and an ESR1 mutation—were the focus of a molecular oncology tumor board session at CAP18.
Read More »AMP case report: Diagnostic pitfalls of testing rare molecular aberrations in lung adenocarcinomas
February 2019—Lung cancer is the second most commonly diagnosed malignancy and results in the most cancer-related deaths each year in the United States, but actionable aberrations in EGFR, ALK, ROS1, and other oncogenes are improving outcomes for a subset of patients.
Read More »Taking measure of cholangiocarcinoma
January 2019—Ten years ago, says Manhal Izzy, MD, the approach might have seemed quixotic: performing liver transplants in patients with early intrahepatic cholangiocarcinoma. Even today, it’s hardly standard of care. Nevertheless, it has moved well beyond the impossible dream category. Medicine advances, and practices change. There’s nothing unusual about that. But Dr. Izzy, assistant professor of medicine, Vanderbilt University School of Medicine, and transplant hepatologist, Vanderbilt University Medical Center, goes out of his way to credit the wisdom and work of those in hepatology and oncology who have been pushing forward curative approaches for cholangiocarcinoma.
Read More »Time now for tumor mutational burden?
November 2018—Like a piece of so-called sticky music, cutoff numbers can persist in physicians’ minds outside of any real clinical value and, in the process, leave their laboratory colleagues mildly befuddled (not to mention searching for more useful cutoffs). Such a jingle is creeping into tumor mutational burden. Lauren Ritterhouse, MD, PhD.
Read More »Fresh incentive to look for Ph-like ALL
October 2018—Cheryl Willman, MD, could hardly believe her eyes. She and her colleagues at the University of New Mexico, working with collaborators from across the U.S. in the NCI TARGET Project, had submitted 100 cases of high-risk pediatric acute lymphoblastic leukemia to British Columbia’s Cancer Agency for RNA sequencing to figure out why patients were doing so poorly, despite treatment with intensive chemotherapy.
Read More »Molecular ‘bucket list’ for renal cancer
September 2018—Leo Tolstoy is not listed as a coauthor on the most recent iteration of The Cancer Genome Atlas on renal cell carcinoma, which focuses on molecular characterization of RCC.
Read More »NGS to take top spot as cancer biomarker testing broadens
June 2018—For biomarker testing and tissue conservation, all roads lead to next-generation sequencing, says Boaz Kurtis, MD, laboratory and medical director of Cancer Genetics in Los Angeles. Dr. Kurtis said, “There’s no other technology platform out there that can provide the amount of data we need today or will need in the future.”
Read More »Clearing the air for electronic cancer checklists
May 2018—Length, cost, variability in vendor support, and lack of consistency have cast a cloud for pathologist users over the CAP’s cancer protocols and the electronic version of those protocols, the electronic cancer checklists. Work is underway to improve the user experience (Nakhleh RE, et al. Arch Pathol Lab Med. 2017;141[9]:1153–1154). Behind that effort is the undeniable: “Structured discrete data, using a controlled vocabulary, can be captured, stored, and reviewed much more readily than data in other formats,” says Mary Edgerton, MD, PhD, vice chair of the CAP’s Pathology Electronic Reporting (PERT) Committee and associate professor of pathology, University of Texas MD Anderson Cancer Center.
Read More »Scoring gastric, GEJ cancers for PD-L1 expression
February 2018—To some ears, perhaps, the scientific method connotes a process that is standardized and unimaginative. But inventions like Velcro, vulcanization, and the microwave—all stemming from accidental discoveries—testify to the role of luck and leaps of intuition in formulating and modifying a hypothesis.
Read More »Molecular tumor board: a patient with ALK– rearranged lung cancer
February 2018—A case of ALK-rearranged lung cancer was the subject of a multidisciplinary molecular tumor board presented last fall at CAP17 by pathologist Laura J. Tafe, MD, and oncologist Benjamin Levy, MD. Together they offered up insights into the tumor genomics of lung cancer with talk of testing guidelines, targeted therapies, resistance mechanisms, and circulating tumor DNA analysis.
Read More »Next-gen sequencing finds further clinical utility in oncology
January 2018—One of the plenary sessions at the 2017 meeting of the Association for Molecular Pathology—“High Impact Molecular Diagnostics for Cancer and Inherited Diseases”—was a virtual mini-course in the latest and most useful applications of next-generation sequencing to detect germline and somatic mutations in cancer. Both speakers zeroed in on the clinical utility of their innovative diagnostic techniques.
Read More »‘Split’ decisions in CNS tumor update
October 2017—Classifying central nervous system tumors has recently become both more complex and easier. Surgical pathologists now have guidance that helps them work through the whys, hows, and what-ifs of using molecular studies when making diagnoses. The 2016 WHO classification for CNS tumors, which has been described as a conceptual and practical advance over the previous incarnation, from 2007, should also help them move closer to precision medicine.
Read More »Revived hopes, fresh challenges with liquid biopsy
October 2017—Until recently, new treatments for stage 4 lung cancer have generally required weighing toxicity against hopes that patients’ average length of survival might be extended by a month or two. But “our expectations are increasing as therapies have improved,” says Geoff Oxnard, MD, thoracic oncologist at Dana-Farber Cancer Institute and assistant professor of medicine at Harvard Medical School. “Patients and doctors are increasingly expecting targeted therapies with dramatic effect and few side effects.”
Read More »AMP case report: Primary pulmonary adenocarcinoma with an unusual molecular profile of the EGFR gene at initial presentation, October 2017
October 2017—CAP TODAY and the Association for Molecular Pathology have teamed up to bring molecular case reports to CAP TODAY readers. AMP members write the reports using clinical cases from their own practices that show molecular testing’s important role in diagnosis, prognosis, and treatment. The following report comes from the University of Massachusetts Medical School-Baystate, Springfield. If you would like to submit a case report, please send an email to the AMP at amp@amp.org. For more information about the AMP and all previously published case reports, visit www.amp.org.
Read More »Advanced parameters offer faster, surer guidance to cancer care
September 2017—After a career spent studying malignancies in the bone marrow and monitoring the effects of chemotherapy on the bone marrow and neoplastic cells contained therein, Cheryl Hirsch-Ginsberg, MD, stepped out from the bone marrow realm and into the faster-paced world of high-volume hematology.
Read More »Hepatic neoplasms—cases, challenges, cautions
July 2017—Kisha Mitchell Richards, MBBS, once took a picture of the ocean as she went around a bend in the road traveling from Negril to Montego Bay in Jamaica. She showed that photo in the second half of a CAP16 session to prepare the audience to shift gears, as she put it, from the first speaker’s talk on medical liver disease (see “Liver injury patterns: pitfalls and pointers,” March 2017) to hers on hepatic neoplasms. “So for me, we are about to go around a bend to things of sheer beauty,” she said, referring to immunohistochemistry stains in the neoplastic liver. “Unfortunately, that which is beautiful to the pathologist is not often great for the patient. That’s our usual practice,” said Dr. Richards, a pathologist at Greenwich Hospital, Yale New Haven Health, Greenwich, Conn.
Read More »Hepatocellular adenoma subtypes—Which is it?
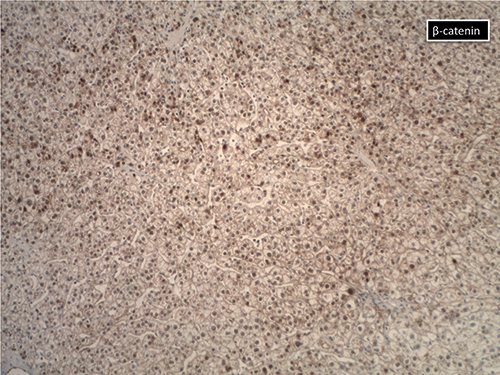
July 2017—Kisha Mitchell Richards, MBBS, a pathologist at Greenwich Hospital, Yale New Haven Health, Greenwich, Conn., recalls that when she was a resident, adenoma was just adenoma. “Nowadays it’s not quite where breast is, where it’s a two-page report, but there are now subtypes of hepatocellular adenomas,” she said in a CAP16 presentation on liver neoplasms. The subtypes are the HNF1 alpha or TCF1 inactivated adenoma, inflammatory adenoma, beta-catenin mutated adenoma, and the unclassified adenoma, which she notes is basically adenoma NOS (not otherwise specified).
Read More »New molecular road map for CRC
April 2017—Molecular testing for colorectal cancer is not for the faint of heart. While that’s not news to Stan Hamilton, MD—he’s head, Division of Pathology and Laboratory Medicine, and the Frederick F. Becker distinguished chair in cancer research, University of Texas MD Anderson Cancer Center—he was reminded of this fact recently when a friend looked at the multipage molecular pathology report on his own tumor.
Read More »In cancer sequencing, a new lingua franca
February 2017—NGS has taken its NBS, or next big step: a newly published joint consensus guideline on how to interpret and report sequence variants in cancer. With these 20 pages of best practices for making next-generation sequencing a regular part of cancer diagnostics, the field is moving, essentially, from frontier town to gated community.
Read More »Guidelines reset horizons of molecular testing in NSCLC
February 2017—It doesn’t happen often. But from time to time, says Gene Finley, MD, director of medical oncology at Allegheny Health Network in western Pennsylvania, a patient who is at death’s door will make such a dramatic recovery with therapy that clinicians refer to it as a “Lazarus effect.”
Read More »AMP case report: An unusual BRAF mutation in a patient with melanoma, February 2017
February 2017—An activating BRAF mutation is found in 40 to 60 percent of melanoma patients. BRAF (B-Raf proto-oncogene) encodes a protein-kinase that activates the MAP kinase/ERK signaling pathway, a pathway that regulates cell differentiation, growth, and survival. Another protein, NRAS, normally activates BRAF. A mutated BRAF, however, can act independently of NRAS and skew cell activity toward growth and survival and away from differentiation.
Read More »Cracking the many mysteries of HER2 GEA
January 2017—Only a sadist would want to see gastroesophageal adenocarcinoma become as common as breast cancer. GEA wreaks enough destruction already as the fifth (stomach) and eighth (esophageal) most common cancers worldwide.
Read More »Highs, lows of immune checkpoint inhibitors
December 2016—Barry Nelson was the first in his cancer patient support group to undergo immunotherapy, which at the time was in a phase one clinical trial at Dana-Farber Cancer Institute. As the therapy became available to others in his group, they would ask for his advice on whether to try it. For the answer, he’d suggest they consult with their doctors and pray. He’d add, “I hope if you decide to go with it that you’ll have the same results that I do.”
Read More »Lymphoid neoplasms: Steven Swerdlow on classification revisions
December 2016—In his CAP16 talk, “Lymphoma Diagnosis and Classification: My Search for the Holy Grail,” Steven H. Swerdlow, MD, acknowledged that the quest has been long and contentious and the resulting classification complex. Why, he asked, is lymphoma classification so complex? It reflects an explosion of knowledge about the immune system and lymphomas and an increasing number of therapeutic targets requiring increasingly precise diagnoses. In other words, it reflects the complexity of the disease itself. As oncologist Alan C. Aisenberg, MD, PhD, wrote in 1995, “The complexity of non-Hodgkin’s lymphoma reflects the complexity of the lymphoid system.”
Read More »Big hopes, bigger questions with PD-L1
November 2016—Progress is a complicated minuet. One popular adage talks of “one step forward, two steps back,” which is not only discouraging but, in an even less-gleaming light, happens to be the title of one of Vladimir Lenin’s books, published in 1904. A more optimistic version (and one less centered on the crisis facing communists in turn-of-the-century Russia) suggests advances occur with two steps forward, mitigated by only one step back.
Read More »Epi proColon fires up hopes of capturing screening dodgers
November 2016—When a Hollywood producer forecasts box office receipts, or a public health official contemplates action against a deadly but preventable cancer, there’s one hypothetical that might make both shudder: What if you held a screening and nobody came?
Read More »Study finds what could be a key to prostate cancer progression
October 2016—The Gleason classification for prostate cancer is by no means going away. But within the Gleason grade, the presence or absence of a DNA-repair gene mutation may signal who is likely to proceed to invasive cancer, says Colin C. Pritchard, MD, PhD, lead author of a study published Aug. 4 in the New England Journal of Medicine.
Read More »For certain thyroid lesions, the shift is on
July 2016—Time was running out for Yuri Nikiforov, MD, PhD, vice chair for molecular pathology and division director of molecular and genomic pathology, University of Pittsburgh Medical Center. For nearly a year he had been working to assemble an international group of experts—pathologists, endocrinologists, a surgeon, and, unusually, a psychiatrist and a patient advocate—to discuss that most vexing of thyroid tumors, encapsulated follicular variant of papillary thyroid carcinoma, or EFVPTC.
Read More »SS18-SSX2 fusion transcript in the diagnosis of a poorly differentiated synovial sarcoma
June 2016—CAP TODAY and the Association for Molecular Pathology have teamed up to bring molecular case reports to CAP TODAY readers. AMP members write the reports using clinical cases from their own practices that show molecular testing’s important role in diagnosis, prognosis, and treatment. The following report comes from Penn State Milton S. Hershey Medical Center and Penn State College of Medicine. If you would like to submit a case report, please send an email to the AMP at amp@amp.org. For more information about the AMP and all previously published case reports, visit www.amp.org.
Read More »Metastatic cancer of unknown primary: diagnostic challenges
May 2016—CAP TODAY and the Association for Molecular Pathology have teamed up to bring molecular case reports to CAP TODAY readers. AMP members write the reports using clinical cases from their own practices that show molecular testing’s important role in diagnosis, prognosis, and treatment. Case report No. 11, which begins here, comes from Cooper Medical School at Rowan University and Cooper University Hospital, Camden, NJ.
Read More »Prostate pointers—PIN, ASAP, mimics, and markers
April 2016—Presenting on prostate cancer diagnosis at CAP ’15 last fall, David G. Bostwick, MD, MBA, recalled how he and Kenneth A. Iczkowski, MD, came up with the term “atypical small acinar proliferation suspicious for but not diagnostic of malignancy,” or ASAP, when they were at Mayo Clinic in 1997. They had scoured the Mayo files trying to spot the right term because they didn’t know what to call it, said Dr. Bostwick, who is medical director of Granger Diagnostics in Richmond, Va. “Should we call it suspicious but not diagnostic? Should we call it worrisome? Problematic?” Dr. Bostwick joked that his favorite expression seen in the files as a prostate biopsy finding in the 1980s was “semi-malignant,” saying, “I still don’t know what that means.”
Read More »The challenge of intraductal carcinoma of prostate
April 2016—In his CAP ’15 presentation last fall, David Bostwick, MD, MBA, referred to intraductal carcinoma of the prostate as “sort of the rage right now in the urologic pathology field.” “The problem is that it has multiple different definitions, and interobserver agreement with it is moderate at best,” said Dr. Bostwick, medical director of Granger Diagnostics in Richmond, Va. Even when pathologists can agree on an IDC diagnosis, he said, they aren’t on the same page about treatment.
Read More »Immunotherapy steers focus to microenvironment
March 2016—It’s not every day that a monoclonal antibody leads the news. But when former president Jimmy Carter was successfully treated for metastasized melanoma last year with the new drug pembrolizumab (Keytruda), the story made headlines. Carter’s recovery—surprising to many when it was announced in December—may have been helped by traditional radiation and chemotherapy. However, the role played by pembrolizumab spotlighted immunotherapy as an exciting advance in the evolution of cancer treatment.
Read More »Community hospitals keep time on tissue handling
February 2016—The great promise of genomics and actionable cancer biomarkers relies on cancer tissues being handled in the right way so they are suitable for study. Reducing cold ischemia time and the total time that biospecimens spend in formalin is key to the process, say guidelines from the CAP and the American Society of Clinical Oncology on HER2 and on estrogen receptor and progesterone receptor testing in breast cancer specimens.
Read More »Non-melanocytic lesions—preventing pitfalls in diagnosis
February 2016—Musician Lauryn Hill has been quoted as saying, “Reality is easy. It’s deception that’s the hard work.” That viewpoint just might resonate with pathologists who sometimes have to diagnose deceiving-looking skin lesions. In a talk at CAP ’15, Deborah L. Cook, MD, professor of pathology and director of dermatopathology at the University of Vermont, shared several case examples that illustrate that investigative effort. All of them involve non-melanocytic malignancies known to mimic benign entities and the converse—“the proverbial wolf in sheep’s clothing” and “sheep in wolf’s clothing,” as she puts it.
Read More »Cases focus on ALK false-negs, post-transplant tumor
January 2016—A sophisticated understanding of the advantages and drawbacks of both familiar and advanced assays can provide great patient benefit, as two talks in a session on solid tumor case studies at the Nov. 5–7, 2015 meeting of the Association for Molecular Pathology showed.
Read More »Prostate biopsy’s role in active surveillance
December 2015—As a treatment option, a strategy of active surveillance is becoming more widely accepted for early stage prostate cancer where risk of progression is low. But the new emphasis on active surveillance brings increased anxiety among prostate cancer patients about the information they’re getting from their physicians and how to deal with it. When M. Elizabeth H. Hammond, MD, participated four years ago in an open dialogue with prostate cancer patients at a conference on active surveillance, “I was really rocked by the things I heard,” she said. “The patients were angry and frustrated by our telling them active surveillance is a good treatment option.
Read More »New guideline spells out IPMN essentials
June 2015—It was a call he dreaded making. It was the late 1990s. Volkan Adsay, MD, was following up on a former patient who had been diagnosed eight years earlier with pancreatic cancer, one related to an intraductal papillary mucinous neoplasm. The patient’s medical record noted that despite chemotherapy, the prognosis was grim.
Read More »Colorectal carcinoma with germline MLH1 promoter hypermethylation
April 2015—CAP TODAY and the Association for Molecular Pathology have teamed up to bring molecular case reports to CAP TODAY readers. Here, this month, is case No. 7.
Read More »Keeping an active eye on prostate cancer
April 2015—In December 2011, M. Elizabeth H. Hammond, MD, was a member of an expert panel for an NIH State-of-the-Science conference on the role of active surveillance in managing men with localized prostate cancer. At these public meetings patients can address the panelists.
Read More »Genetic profiling vies with IHC in retune of CUP testing
March 2015—Tesla beats Camry. Online catalogs replace paper. Keurig edges out Chemex. Mobile trounces landline. When paradigms shift, the theory goes, we can only cling to the technology in the outbox for just so long. But that’s a theory that may not apply to diagnostic testing for cancer of unknown primary (CUP). Microarray-based gene expression profiling (GEP) has recently gained a foothold in the quest to identify origins and therapeutic targets for metastatic cancer, but traditional immunohistochemistry is not about to be sidelined.
Read More »Coag quest: keying into the clot risk of cancer patients
January 2015—It’s a somewhat stark fact: When hospitalized cancer patients die from something other than cancer, the cause is most likely to be venous thromboembolism. But there is a degree of mystery about why some cancer patients are more prone than others to be afflicted with VTE.
Read More »Thyroid cancer: In a flourish of subtypes, genes, and drivers
January 2015—Dark matter is shrinking—at least in the thyroid cancer part of the universe. Until recently, the percentage of papillary thyroid carcinomas with no known oncogenic drivers hovered around 25 percent. Now, with the publication of the most recent research effort by The Cancer Genome Atlas project, that number has shrunk considerably, to about 3.5 percent.
Read More »AML molecular testing a map with many paths
July 2014—When it comes to molecular testing for acute myeloid leukemia, the approach seems more Montessori than military school. There are some basic steps physicians should take, to be sure. Cytogenetics still shepherds patients into three prognostic groups: favorable, intermediate, and unfavorable. And several gene mutations—NPM1, CEBPA, FLT3, and KIT—alone or in combination, and with various cytogenetic associations, provide additional prognostic and therapeutic guidance.
Read More »Data spark new directions in cervical cancer
June 2014—When Mark Stoler, MD, stood up to speak at the 30th annual Clinical Virology Symposium on April 29, his topic was timely. Dr. Stoler was presenting three-year followup data from the ATHENA trial, in which a primary human papillomavirus screening algorithm based on the Roche Cobas HPV assay was compared with traditional cytology and a hybrid cotesting algorithm for their ability to prevent cervical cancer.
Read More »Cancer biomarker use varies widely, needs a ‘broader view’
June 2014—Despite an explosion of research into cancer biomarkers and professional guidelines that urge testing for certain genetic mutations that help detect disease, anticipate its course, or predict response to treatment, many cancer centers are out of sync with oncology testing recommendations. Payment policies, regulatory oversight, clinician preferences, and varying access to testing technology are among the factors that contribute to discrepancies in cancer care.
Read More »Second act for HER2, in gastric cancers
May 2014—If one were to map out a “family tree” of tumors, breast and gastric cancers might end up looking like second cousins. One is common, the other is not, but it’s rapidly becoming known that they share a kinship of sorts with HER2 testing and the targeted therapy trastuzumab.
Read More »Unraveling metastasis with circulating tumor cells
May 2014—Some diseases have clear origins and unfold in predictable ways, but cancer isn’t one of them. Despite legions of studies over the decades, cancer tumorigenesis and its deadly sequel, metastasis, essentially remain a riddle, wrapped in a mystery, inside an enigma, as Winston Churchill once described Russia.
Read More »MicroRNA markers show staying power
March 2014—Not many components of human cell biology have been discovered and immediately dubbed “junk.” But micro-RNAs, small noncoding RNA molecules first identified in 1993, fall into that category. Like Hans Christian Andersen’s Ugly Duckling, microRNAs began their life after discovery with people scoffing at them. People even laughed at researchers who thought microRNAs held promise in diagnosing cancer.
Read More »HPV a game changer in head, neck tumors
December 2013—Not that any cancer is ever “easy,” but until relatively recently, the culprit in head and neck squamous cell carcinomas was clear. The vast majority were caused by “smoking, smoking, and smoking,” says William Westra, MD, professor of pathology, oncology, and otolaryngology/head and neck surgery, and associate director, surgical pathology, The Johns Hopkins Medical Institutions. Call this HNSCC’s antediluvian era.
Read More »No worries with new cancer biomarker templates
October 2013—For anyone worried about the new CAP reporting templates for cancer biomarkers, Patrick L. Fitzgibbons, MD, has an important message: Don’t panic. “These are nothing new,” says Dr. Fitzgibbons, a pathologist at St. Jude Medical Center, Fullerton, Calif., and chair of the CAP Cancer Biomarker Reporting Committee. “We’re not adding anything. The templates will look very familiar to users of the CAP cancer protocols. They shouldn’t be considered a significant burden.”
Read More »New guideline takes on tough HER2 cases
October 2013—In HER2 testing for breast cancer, the term “equivocal” verges on being a four-letter word. If the patient has a clearly positive test result, therapies targeting HER2 become a treatment option, and a highly successful one at that. If the result is clearly negative, HER2-targeting drugs are off the table; the patient isn’t expected to benefit from the drugs, which are expensive and can be cardio- toxic.
Read More »ALK-positive NSCLC—patient’s story opens eyes
September 2013—For good or bad, Matthew Hiznay seems to be an odds beater. First, a minority of lung cancer patients have never smoked. He’s one of them, having been diagnosed with late-stage non-small-cell lung cancer in August 2011. Obviously, that’s the bad.
Read More »AMP case report: aCGH as a diagnostic aid in a childhood Spitzoid melanoma
September 2013—CAP TODAY and the Association for Molecular Pathology have teamed up to bring molecular case reports to CAP TODAY readers. Here, this month, is the third such case. (See the February 2013 issue for the first, on multilocus sequencing for rapid identification of molds, and last month’s issue for the second, on the importance of screening for Lynch syndrome in patients with endometrial cancer.)
Read More »Cytopathology and More | Managing abnormal screening results: highlights of new guidelines
August 2013—The field of cervical cancer screening saw many developments in 2012. In April last year, the American Cancer Society, American Society for Colposcopy and Cervical Pathology, and American Society for Clinical Pathology published new guidelines for cervical cancer screening, most notably raising the age at which screening should begin, extending the interval between screening tests, and giving preference to simultaneous Pap and human papillomavirus co-testing in women ages 30 to 65.1 Almost simultaneously, the U.S. Preventive Services Task Force published similar screening guidelines.2 Then, in July, the CAP and ASCCP published the results of a joint project recommending a uniform Lower Anogenital Squamous Terminology (LAST).3 Finally, in September the ASCCP led a consensus conference of 23 participating organizations to update guidelines for managing abnormal cervical cancer screening test results. In April of this year, these updated guidelines were published simultaneously in the Journal of Lower Genital Tract Disease and Obstetrics and Gynecology.4,5
Read More »Molecular clonality testing for lymphoma
May 2013—Most jobs in the kitchen or the home workshop can be done with a basic set of tools. But every once in a while you need something special—a zester, say, or a dremel—and in those situations it’s nice to have that special tool on hand. Even more important, it’s nice to know how to use it.
Read More »New guidance on lung cancer testing
April 2013—It was a monumental task: create a molecular testing guideline for lung cancer. Among other tasks, those involved (representing the CAP, the International Association for the Study of Lung Cancer, and the Association for Molecular Pathology) reviewed 1,533 abstracts and read, in detail, 521 full-text articles. There was extensive evidence grading; naturally, new literature was published in the interim, which required even more reviews. The payoff was the first international, evidence-based, multidisciplinary guideline for this part of lung cancer care. It contains 37 items addressing 14 subjects, including 15 recommendations (evidence grade A/B).
Read More » CAP TODAY Pathology/Laboratory Medicine/Laboratory Management
CAP TODAY Pathology/Laboratory Medicine/Laboratory Management