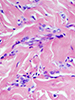
April 2016—Presenting on prostate cancer diagnosis at CAP ’15 last fall, David G. Bostwick, MD, MBA, recalled how he and Kenneth A. Iczkowski, MD, came up with the term “atypical small acinar proliferation suspicious for but not diagnostic of malignancy,” or ASAP, when they were at Mayo Clinic in 1997. They had scoured the Mayo files trying to spot the right term because they didn’t know what to call it, said Dr. Bostwick, who is medical director of Granger Diagnostics in Richmond, Va. “Should we call it suspicious but not diagnostic? Should we call it worrisome? Problematic?” Dr. Bostwick joked that his favorite expression seen in the files as a prostate biopsy finding in the 1980s was “semi-malignant,” saying, “I still don’t know what that means.”
Read More »The challenge of intraductal carcinoma of prostate
April 2016—In his CAP ’15 presentation last fall, David Bostwick, MD, MBA, referred to intraductal carcinoma of the prostate as “sort of the rage right now in the urologic pathology field.” “The problem is that it has multiple different definitions, and interobserver agreement with it is moderate at best,” said Dr. Bostwick, medical director of Granger Diagnostics in Richmond, Va. Even when pathologists can agree on an IDC diagnosis, he said, they aren’t on the same page about treatment.
Read More »Non-melanocytic lesions—preventing pitfalls in diagnosis
February 2016—Musician Lauryn Hill has been quoted as saying, “Reality is easy. It’s deception that’s the hard work.” That viewpoint just might resonate with pathologists who sometimes have to diagnose deceiving-looking skin lesions. In a talk at CAP ’15, Deborah L. Cook, MD, professor of pathology and director of dermatopathology at the University of Vermont, shared several case examples that illustrate that investigative effort. All of them involve non-melanocytic malignancies known to mimic benign entities and the converse—“the proverbial wolf in sheep’s clothing” and “sheep in wolf’s clothing,” as she puts it.
Read More »Prostate biopsy’s role in active surveillance
December 2015—As a treatment option, a strategy of active surveillance is becoming more widely accepted for early stage prostate cancer where risk of progression is low. But the new emphasis on active surveillance brings increased anxiety among prostate cancer patients about the information they’re getting from their physicians and how to deal with it. When M. Elizabeth H. Hammond, MD, participated four years ago in an open dialogue with prostate cancer patients at a conference on active surveillance, “I was really rocked by the things I heard,” she said. “The patients were angry and frustrated by our telling them active surveillance is a good treatment option.
Read More »28 given awards for notable and longtime service
November 2015—Donald S. Karcher, MD, was presented Oct. 4 with the Pathologist of the Year award during the spotlight event at the CAP ’15 annual meeting in Nashville. At the same event, at the Gaylord Opryland, Rajesh C. Dash, MD, was given the Pathology Advancement award, and Latha Pisharodi, MD, received the CAP Foundation Gene and Jean Herbek Humanitarian award. Mary L. Paton, MT(ASCP), was given the CAP Staff Outstanding Achievement award.
Read More »At CAP ’15, 98 courses and a focus on daily practice
May 2015—With several dozen pathology associations worldwide, many with their own meetings, why should a pathologist opt to attend CAP ’15 in Nashville, Tenn., Oct. 4–7? Philip Cagle, MD, supplies some thoughts. “There are many pathology organizations, and each has its own niche. Whereas at the CAP meeting, there are many courses covering a broad range of areas, from things such as practice management and quality assurance to different areas of anatomic pathology and clinical pathology,” says Dr. Cagle, ...
Read More » CAP TODAY Pathology/Laboratory Medicine/Laboratory Management
CAP TODAY Pathology/Laboratory Medicine/Laboratory Management