Editor: Frederick L. Kiechle, MD, PhD
Submit your pathology-related question for reply by appropriate medical consultants. CAP TODAY will make every effort to answer all relevant questions. However, those questions that are not of general interest may not receive a reply. For your question to be considered, you must include your name and address; this information will be omitted if your question is published in CAP TODAY. Submit a question.
Q. Insulin assays traditionally have been used to work up hypoglycemia, but we are noticing more and more requests for insulin and C-peptide testing. Is there a reason for this shift?
A. July 2024—It is well established that the prevalence of diabetes has been steadily increasing over the past 20 years. The Centers for Disease Control and Prevention reports that in 2021, an estimated 11 percent of the U.S. population, or 38.4 million people, had diabetes.1 Therefore, clinical laboratories may be seeing an uptick in insulin and C-peptide testing.
Testing guidelines for diagnosing and managing type 1 and type 2 diabetes in children and adults recommend measuring C-peptide in certain circumstances but do not recommend routinely measuring insulin. Therefore, any uptick in insulin testing should be reviewed closely for possible misutilization of the test, as providers may be inappropriately defaulting to paired ordering of these analytes.
“Standards of Care in Diabetes—2024,” published by the American Diabetes Association, recommends measuring C-peptide when the initial clinical presentation of diabetes is not clearly diagnostic for type 1 versus type 2. When classification is unclear and islet autoantibody testing is negative, C-peptide testing while the patient is on insulin therapy can be used to differentiate type 1 from type 2 diabetes.2
C-peptide levels below 200 pmol/L are indicative of type 1 diabetes and levels above 600 pmol/L are indicative of type 2 diabetes. Intermediate C-peptide levels (between 200 and 600 pmol/L) may occur in people with monogenic diabetes, which can be confirmed through genetic testing, or may result in an indeterminate diabetes classification, with the recommendation to repeat C-peptide testing after five or more years.
Guidelines on laboratory analysis in diabetes published through a collaboration between the Association for Diagnostics and Laboratory Medicine (formerly AACC) and ADA recommend measuring a fasting C-peptide level as a reflex test when the fasting plasma glucose is ≤ 220 mg/dL (12.5 mmol/L) only if C-peptide testing is required by insurance to cover payment for an insulin pump.3 The guidelines also state that measuring insulin in people who are at risk for or have diabetes is not recommended and that insulin measurement should be reserved for research purposes.3 Neither insulin nor C-peptide testing should be used to assess insulin resistance in women with polycystic ovarian syndrome.
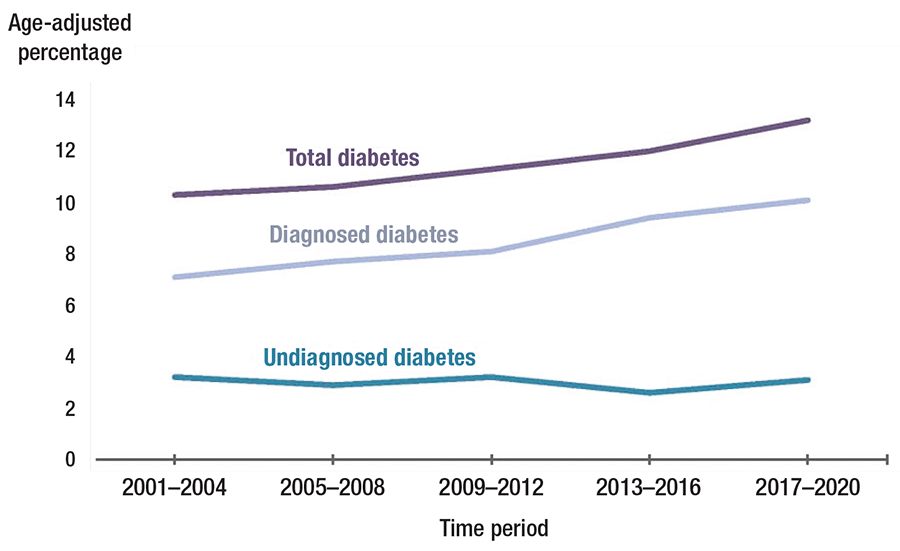
Data sources: 2001–March 2020 National Health and Nutrition Examination Surveys. Source: CDC. The figure is available on the CDC website for no charge. Its use does not constitute an endorsement or recommendation by the U.S. government, Department of Health and Human Services, or Centers for Disease Control and Prevention.
In summary, paired measurement of insulin and C-peptide should be reserved for assessing patients with nondiabetic hypoglycemia, which is a relatively uncommon diagnosis secondary to a variety of rare etiologies. Increases in testing volume for C-peptide could be the result of the uptick in diabetes rates, as C-peptide testing may be needed to distinguish between type 1 and type 2 diabetes if the clinical presentation is ambiguous or to provide insurers with evidence of the need for insulin pump therapy. Measuring insulin in patients with diabetes is not recommended. Clinical laboratory directors should investigate increases in testing volume for insulin, as misutilization is likely.
- National Diabetes Statistics Report. Centers for Disease Control and Prevention. Jan. 8, 2024. www.cdc.gov/diabetes/php/data-research/?CDC_AAref
- American Diabetes Association Professional Practice Committee. 2. Diagnosis and classification of diabetes: standards of care in diabetes—2024. Diabetes Care. 2024;47(suppl 1):S20–S42.
- Sacks DB, Arnold M, Bakris GL, et al. Guidelines and recommendations for laboratory analysis in the diagnosis and management of diabetes mellitus. Clin Chem. 2023;69(8):808–868.
Amy B. Karger, MD, PhD, DABCC
Medical Director, West Bank Laboratory
System Director, Point-of-Care Testing
Director, Biochemical Genetics Laboratory
M Health Fairview
Professor, Department of Laboratory Medicine and Pathology
University of Minnesota
Member, CAP Accuracy-Based Programs Committee
Sridevi Devaraj, PhD, DABCC
Medical Director, Clinical Chemistry and Point of Care Testing
Texas Children’s Hospital and Pavilion for Women
Director of Laboratories
Center for Women and Children
Texas Children’s Health Plan
Professor, Pathology and Immunology
Baylor College of Medicine
Houston, Tex.
Member, CAP Accuracy-Based Programs Committee
Q. How should a lot-to-lot formalin comparison be done?
A. CAP anatomic pathology checklist requirement ANP.10041 Quality of Formalin requires laboratories to “monitor the quality of formalin provided for fixation of specimens to be submitted for pathology and for use as a fixative in the laboratory.”
Laboratories that mix their own formalin need to check and record the pH to ensure the formalin is mixed correctly. Laboratories that purchase formalin ready for use can spot-check new lots for pH level or retain records of the manufacturer’s quality control certificate. Laboratories are not required to perform comparison studies of new versus old lots of formalin.
College of American Pathologists. ANP.10041 Quality of formalin. In: Anatomic pathology checklist. Aug. 24, 2023.
O’Leary TJ, Fowler CB, Evers DL, Mason JT. Protein fixation and antigen retrieval: chemical studies. Biotech Histochem. 2009;84(5):217–221.
Thavarajah R, Mudimbaimannar VK, Elizabeth J, Rao UK, Ranganathan K. Chemical and physical basics of routine formaldehyde fixation. J Oral Maxillofac Pathol. 2012;16(3):400–405.
Christina Bowerman, MLS(ASCP)
Technical Specialist
Laboratory Accreditation Services
College of American Pathologists
Northfield, Ill.

