Suzanne Crumley, MD
Sinchita Roy-Chowdhuri, MD, PhD
Kaitlin Sundling, MD, PhD
January 2022—A consistent virtue of the cytopathology laboratory is that it combines two qualities essential to patient care: It provides an accurate and timely diagnosis. The ability to make a prompt diagnosis is particularly important in immunosuppressed or otherwise vulnerable patient populations for whom a timely diagnosis can result in early treatment initiation and potentially better outcomes.
Cytopathology laboratories that serve immunosuppressed patients frequently encounter bronchoalveolar lavage (BAL), bronchial washing, bronchial brushing, or cerebrospinal fluid specimens that are submitted to exclude bacterial, viral, fungal, and mycobacterial infections. If an infectious etiology is suspected, these specimens are likely to also have concurrent microbiological cultures submitted.
However, the ability to use special stains on cytologic preparations may increase the rapidity of diagnosis. In cases in which malignancy was suspected, material for microbiologic cultures may not have been collected upfront, making timely and accurate cytologic diagnosis of organisms even more important. Cytospins or ThinPreps can typically be made and stained within hours or the same day, rather than require the more time-consuming process needed for cell block preparation and formalin fixation. For these reasons, special stains such as Grocott methenamine silver (GMS), periodic acid-Schiff-diastase (PASD), mucicarmine, or acid-fast bacilli (AFB), among others, may be ordered by the cytopathologist or clinical team on cytologic preparations.
The diagnosis of Pneumocystis jirovecii (carinii) infection is an exemplar of the value of special stains in cytology, as this organism cannot be cultured in the microbiology laboratory. Additional examples, such as early identification of Histoplasma sp., Aspergillus sp., Coccidiodes sp., Cryptococcus sp., and Mucor sp., abound in cytology and are not limited to respiratory tract specimens, as cerebrospinal fluid and other body sites sampled by cytology may harbor fungal or mycobacterial infections. We have shown that cytopathologists can diagnose unsuspected mycobacterial infections, resulting in earlier treatment and appropriate patient isolation.1
Although a perfect correlation between cytology and microbiology culture is not attainable, as the Houston Methodist Hospital (HMH) cytology practice and others have shown (particularly with regard to fungal morphology),2-4 cytology can provide an early narrowing of the differential diagnosis, allowing for empiric treatment while microbiological cultures are in progress.
The HMH cytology laboratory provides the option to order a BAL with or without additional GMS special stain, which is performed on two additional cytospins. A BAL with GMS is essentially always requested for lung transplant patients and can also be ordered in other patients upon clinician or cytopathologist request, making this a high-volume order on cytology at our institution. The HMH cytology laboratory currently performs more than 2,200 GMS special stains per year on cytologic preparations. There has been debate about the cost-benefit analysis of reflex GMS testing on BAL specimens.5,6 However, other institutions have found that reflex GMS testing on the BAL specimens from lung transplant patients is of benefit, supporting this ordering practice.7
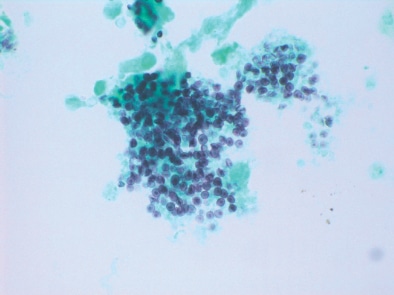
How do we ensure that the special stains performed on cytology specimens are performed consistently and accurately? There are some differential considerations based on the preparation type (such as ThinPrep, cytospin, cell block) and whether the stain of interest is a special/histochemical stain (such as GMS, AFB, or PAS) or immunohistochemical (such as IHC for Treponema pallidum, cytomegalovirus, BK virus, or other specific organisms).
Depending on the preparation type, there are specific challenges to validation and control methodologies for cytology as compared with surgical pathology. Cytologic collections from the respiratory tract, and from the CSF, are usually low-volume specimens with a limited shelf-life. Having readily available identical cytologic control specimens for identification of Pneumocystis sp. is particularly difficult because this is not an especially frequent diagnosis, the organisms cannot be grown in a culture, and even the positive cases may have only a few viable fungi.
The most commonly ordered special stain in the HMH cytopathology laboratory is the GMS stain. The GMS control specimens are performed for each batch of stains performed, with review and verification of the control by the cytopathologist on service prior to reporting. At HMH, the control specimens used are of the similar cytologic specimen type if available; if not, positive surgical pathology tissue samples are used for the daily batched workflow. This fulfills the requirements for daily verification of special stain quality on cytology and mirrors the similar practice for surgical pathology specimens.
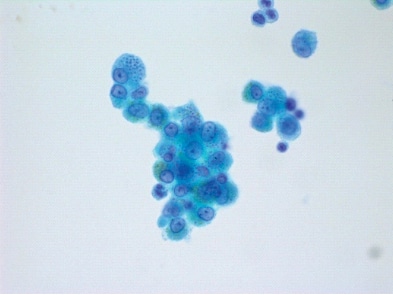
If the special stains are performed on cell block preparations, the CAP accreditation checklists define that the validation, as well as verification of positive and negative controls, are regulated under the anatomic pathology checklist. While cell block preparations are more histology-like and have a long shelf-life, they may be handled and processed differently from surgical biopsy specimens, with a prominent difference being the potential for prefixation in alcohol. If cell blocks will be stained routinely for microbiologic organisms, it may be prudent to include them in the initial validations of the appropriate special stains.
The methodology for initial validation of special stains in cytology may depend on their frequency of use, and the current discussion does not address all the nuances pertinent to each laboratory. Best practices and regulatory requirements are better defined for immunohistochemistry on cytologic preparations, which are discussed in detail in the CAP principles of analytic validation of immunohistochemical assays8 and within the most recent version of the CAP cytopathology checklist.
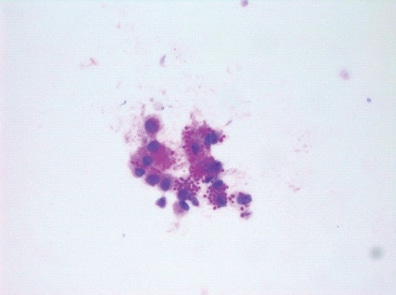
In conclusion, examination of special stains in cytology is particularly prescient in the current era, with a larger pool of immunosuppressed patients owing to COVID-19 diagnoses and treatment, and unfortunately also including additional lung transplant recipients post-COVID-19 diagnosis. The cytology laboratory has always had an important role to play in early diagnosis and treatment for infectious processes, and cytopathologists should understand how to appropriately use and maintain a high-quality special stain on cytologic preparations. Although the special stain may perhaps be considered to be old-fashioned and humble, as compared with the more recent evolution of immunohistochemical stains, it continues to be mighty.
- Suo L, Sheu TG, Crumley SM. Mycobacterium tuberculosis diagnosed promptly by bronchial brushing cytology in an immunocompetent patient. Diagn Cytopathol. 2020;48(4):368–370.
- Crumley S, Hull A, Cernoch P, Mody D, Sneige N. Comparison between cytologic examination of fungi in bronchial washings and bronchoalveolar lavage specimens and culture: a review of 100 cases with emphasis on diagnostic pitfalls. J Am Soc Cytopathol. 2014;3(4):211–217.
- Sangoi AR, Rogers WM, Longacre TA, Montoya JG, Baron EJ, Banaei N. Challenges and pitfalls of morphologic identification of fungal infections in histologic and cytologic specimens: a ten-year retrospective review at a single institution. Am J Clin Pathol. 2009;131(3):364–375.
- Guarner J, Brandt ME. Histopathologic diagnosis of fungal infections in the 21st century. Clin Microbiol Rev. 2011;24(2):247–280.
- Lang-Orsini M, Genega EM, Bedrossian K, Roychowdhury M. Empirical ordering of stains in cytology—are we saving or losing? J Am Soc Cytopathol. 2021;10(6):585–591.
- Nassar A, Zapata M, Little JV, Siddiqui MT. Utility of reflex gomori methenamine silver staining for Pneumocystis jirovecii on bronchoalveolar lavage cytologic specimens: a review. Diagn Cytopathol. 2006;34(11):719–723.
- Torous VF, Pitman MB, Ly A. Evaluation of the clinical utility of reflex GMS and AFB stains on BAL specimens from lung transplant patients. J Am Soc Cytopathol. 2020;9(3):166–172.
- Fitzgibbons PL, Bradley LA, Fatheree LA, et al. Principles of analytic validation of immunohistochemical assays: guideline from the College of American Pathologists Pathology and Laboratory Quality Center. Arch Pathol Lab Med. 2014;138(11):1432–1443.
Dr. Crumley is assistant professor at Houston Methodist Hospital, Dr. Roy-Chowdhuri is associate professor at the University of Texas MD Anderson Cancer Center, and Dr. Sundling is assistant professor at the University of Wisconsin. All are members of the CAP Cytopathology Committee.

