From the CAP Cytopathology Committee;
Jordan Paul Reynolds, MD, Derek B. Allison, MD, Editors
Janie Roberson, SCT(ASCP)
Donna K. Russell, MEd, CT(ASCP)
Dawn Underwood, MEd, CT(ASCP)
Sana Tabbara, MD; Shahla Masood, MD
Diane D. Davey, MD
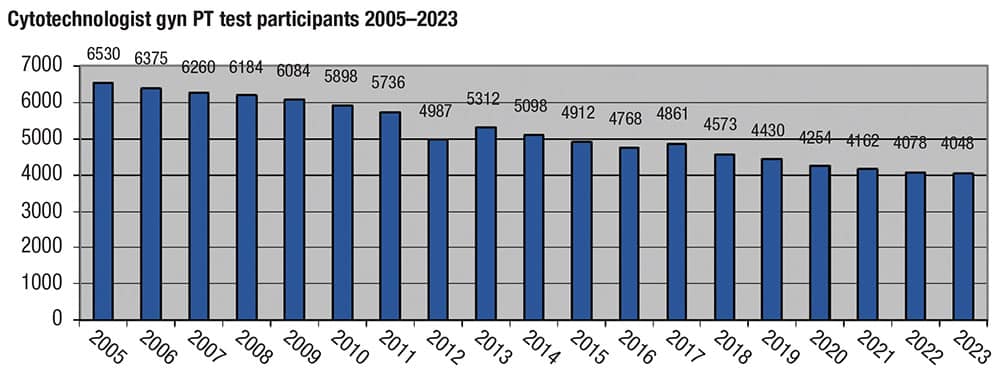
January 2025—It is well documented that the cytologist/cytotechnologist workforce is diminishing and the number of training programs has declined. According to the Centers for Medicare and Medicaid Services,1 CT participation in gynecologic proficiency testing has decreased by 27 percent since 2005 (Fig. 1). New board certifications of CTs or specialists in CT(SCT) decreased by about 56 percent over the same period. CT(ASCP) and all SCT(ASCP) certifications are now recognized by the CMS and the Centers for Disease Control and Prevention per 42 CFR §493.1483.2
A 2023 cytology employment survey conducted by the American Society for Cytotechnologists and distributed by the ASCT and American Society for Clinical Pathology found high anticipated retirement rates comparable to those reported over the past several years (publication pending). This survey showed vacancy rates are projected to continue to increase over the next five years. As a result, staffing shortages will continue and worsen. However, opportunities exist for the creation of skills-based competencies that engage practicing CTs, facilitate career advancement, and mitigate job burnout. Laboratories involved in training, including affiliate sites, will continue to elevate the skills and expertise of CTs. Importantly, the current reported scope of practice in the field shows CTs are advancing the profession, and salaries are increasing modestly across all cytology position categories. The interest in cytology has therefore been elevated and many programs are seeing additional applicants.
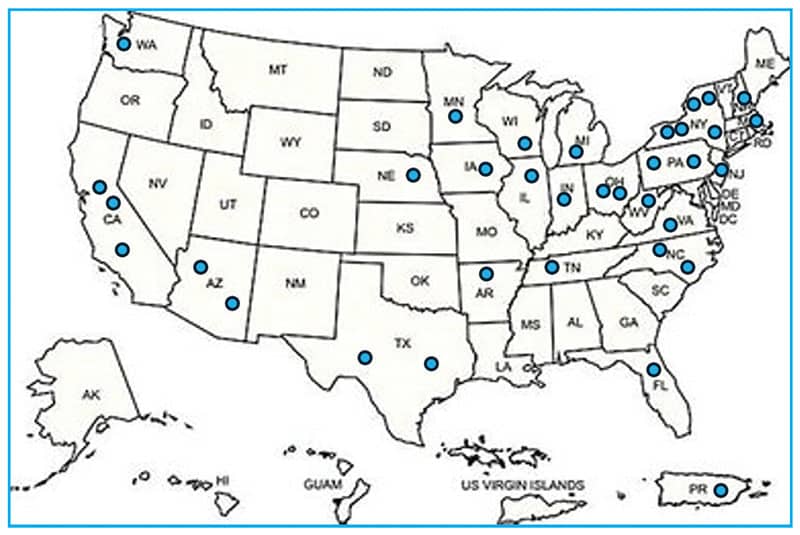
Eighteen programs are currently accredited by the Commission on Accreditation of Allied Health Education Programs. This may appear to limit geographic locations where hospitals and laboratories can be clinically affiliated with a program, but many CT training programs use distance education and online teaching modalities. Students can learn at multiple clinical placement locations that operate under a single training program (Fig. 2). The University of Nebraska program has clinical placement agreements in 17 states, and Albany College of Pharmacy and Health Sciences has expanded to two satellite sites. Recent student enrollment was reported at the Strategies in Education session at the American Society of Cytopathology annual scientific meeting in November 2024, noting an increase to 182 students enrolled. This expansion is largely due to the innovative satellite and placement strategies.
The ASC Cytology Programs Review Committee is recognized as an accreditation committee of the Commission on Accreditation of Allied Health Education Programs. The review committee is responsible for the ongoing review of all training programs to ensure compliance with standards, and it supports the programs by providing educational resources and promoting collaboration among programs. Review committee membership consists of representatives appointed by four sponsoring societies with interest in cytology education, including the CAP.
The cytology community is actively engaged in aligning training with practice as well as increasing the educational level to Master’s degrees. Currently the 18 programs located in the United States and Puerto Rico represent eight certificate-only programs, four Bachelor’s-degree-only programs, five Master’s-degree-only programs, and one dual degree (Bachelor’s/Master’s) program. The review committee’s new standards and guidelines take effect this month, January 2025, but existing programs have additional years to convert to Master’s programs. While most institutions lack the resources to develop or sustain a training program, becoming a clinical affiliate site may be an attainable and beneficial goal. The purpose of this article is to highlight some of the benefits and expectations of this important collaboration.
Mutual benefits. Clinical affiliations may range from two-week or longer clinical rotations or may involve serving as a clinical placement or satellite site. More substantial affiliations such as placing learners in another state require additional paperwork including review committee approvals. Each program (including a placement site or satellite) may have up to several clinical rotations in different hospitals or laboratory settings, or include sites where students have an interest.
Clinical affiliations offer numerous benefits to the clinical affiliate, including supporting the profession nationally and addressing workforce gaps in areas lacking regional training programs. Hosting students requires additional effort, but it provides a unique opportunity to evaluate their skills and work habits and thus serves as an extended job interview. Many staff members find mentoring students rewarding, as it enriches the workday and fosters informal teaching opportunities. This arrangement also allows the laboratory to assess whether a student would be a strong fit for its cytology team.
Students benefit from clinical rotations by gaining firsthand exposure to different laboratory environments such as reference laboratories, hospitals, academic institutions, or other specialized settings. This experience allows them to evaluate which type of workplace best aligns with their career goals while they also immerse themselves in the laboratory’s culture. In essence, rotations serve as a trial period to determine if the site is a good mutual fit for future employment.
Training programs benefit by expanding student placement options and accommodating a variety of workplace settings across diverse geographic areas. The growing use of distance learning further enhances these opportunities, enabling programs to partner with high-level academic institutions and provide students with access to cutting-edge technologies.
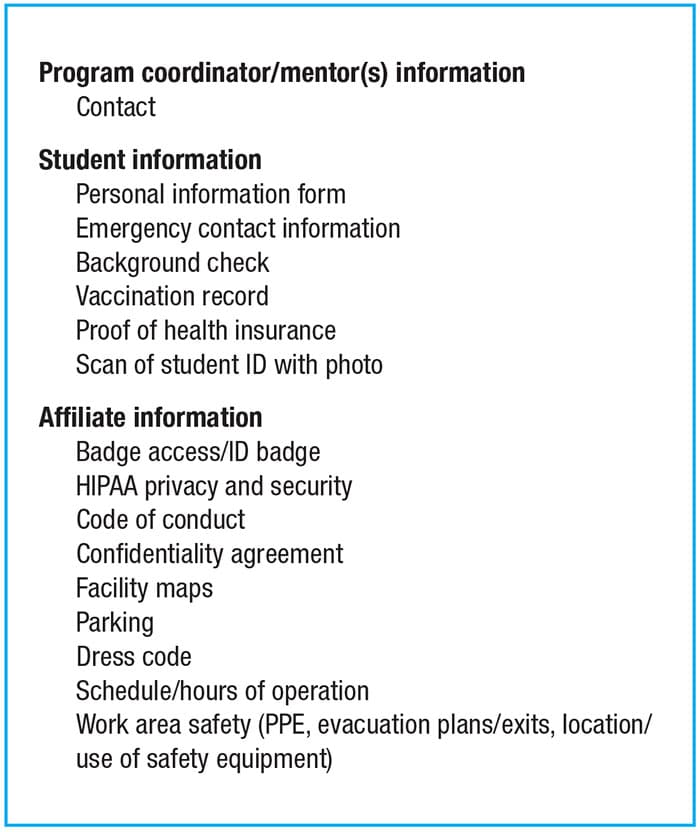
What makes a good clinical affiliate? There are tangible and intangible requirements for a successful clinical affiliation. A student “mentor” should be identified for key communications among the parties, and a student orientation checklist should be developed to cover essential information (Fig. 3). Most institutions will require a contract or affiliation agreement between the institutions. This agreement typically includes documentation requirements for background checks, health insurance, and basic student competencies. From a practical standpoint, students should know details in advance, including dress code, parking options, and hours of operation.
Test volumes, case diversity, facilities, and equipment should be sufficient to ensure a comprehensive and enriching learning experience for students. Essential components of training include rapid on-site assessments conducted under pathologist supervision, gross examination and tissue submission of small biopsies, imaging techniques, and exposure to telecytology and digital scanning technologies. These practices align with the new entry-level competencies and provide valuable, practical training opportunities. Additionally, all required training documentation should be completed and provided to the student for reference and compliance.
As an intangible, the laboratory culture should be encouraging and accepting of trainees. Laboratory staff should be informed of the expectations and encouraged to be mentors to and welcoming, positive role models for students.
How can training programs best interact with and recruit clinical affiliates? Training programs should ensure that the student is ready and competent for a clinical rotation that fits efficiently into the laboratory work setting. The training program should meet with the affiliate to discuss expectations for the student while they complete the clinical affiliate training. Students will often have capstone projects or other weekly assignments to complete during the affiliate training and thus they may need dedicated time to complete the cytology program requirements.
Affiliate recruitment may be performed locally or nationally. Programs can offer a mix of affiliate setting sites to include private laboratories, academic institutions, cancer centers, and community hospital laboratories. If a student would like to return to their home state for employment, it may be advantageous to recruit affiliate sites from that area. Laboratories may invest the time as an affiliate training site if they can employ the student upon graduation from the cytology training program.
Conclusion. The laboratory workforce faces significant challenges on a national scale, with the cytology field grappling with unique issues such as evolving technologies, shifting cervical cancer screening guidelines, and a transforming workforce. Although CT training programs are relatively few, the cytology community has a wealth of outstanding institutions and talented CTs and pathologists to enhance training opportunities. The profession is well positioned to work together for the mutual benefit of students, employers, and the patients we ultimately serve. Hospitals and laboratories interested in serving as a clinical affiliate are encouraged to contact CT training programs. Additional information including contact information for accredited programs can be found through the Commission on Accreditation of Allied Health Education Programs and the American Society of Cytopathology websites in the reference list below.3-5
- Cytology Proficiency Testing Results—Initial Test 2005 to 2023. Centers for Medicare and Medicaid Services. https://www.cms.gov/files/document/cytology-pt-results-2005-2023.pdf
- American Society for Clinical Pathology (ASCP) Board of Certification (BOC) Specialist in Cytology (SCT) as an Approved Board Certification for the Clinical Laboratory Improvement Amendments (CLIA) for Individuals Performing Testing in the Subspecialty of Cytology. Centers for Medicare and Medicaid Services. July 8, 2024. https://www.cms.gov/files/document/admin-info-24-16-clia.pdf
- Find an accredited program. Commission on Accreditation of Allied Health Education Programs. https://caahep-public-site-5be3d9.webflow.io/students/find-an-accredited-program
- Cytology Programs Review Committee. Commission on Accreditation of Allied Health Education Programs. https://caahep-public-site-5be3d9.webflow.io/committees-on-accreditation/cytology
- Cytology programs. American Society of Cytopathology. https://cytopathology.org/page/CytologyPrograms
Janie Roberson is a cytotechnologist consultant, University of Alabama at Birmingham. Donna Russell is education coordinator of cytopathology residency/fellowship education at UR Medicine and program director of the Daemen University/Roswell Park Comprehensive Cancer Center, Buffalo, NY. Dawn Underwood is manager of cytology, Cleveland Clinic. Dr. Tabbara is senior member and director of cytopathology, Moffitt Cancer Center, and professor of oncologic sciences, USF Health Morsani College of Medicine, Tampa, Fla. Dr. Masood is professor and chair, Department of Pathology and Laboratory Medicine, University of Florida College of Medicine—Jacksonville, and medical director of the UF Health Jacksonville laboratories and UF Health Breast Center. Dr. Davey is professor emerita, University of Central Florida, and pathologist, Orlando VA Medical Center. Dr. Tabbara is advisor to and immediate past chair of the CAP Cytopathology Committee; all other authors are current or past members of the Cytopathology Committee.

