Varsha Manucha, MD
Diane D. Davey, MD
August 2022—The ability to make a definitive diagnosis of mesothelioma on pleural fluid cytology has been questioned and debated for a long time. The 2018 American Society of Clinical Oncology clinical guidelines limit the cytological diagnosis of pleural fluid specimens only as an initial screening test for mesothelioma. Monaco, et al.,1 discuss in their article the appropriate use of ancillary studies (immunohistochemistry and fluorescence in situ hybridization studies) to make a definitive diagnosis of mesothelioma in small tissue samples, which are often processed as cell blocks.
The authors recommend a stepwise approach starting with immunohistochemistry for BAP1 and, next, MTAP in cases of atypical mesothelial proliferations where the suspicion for malignant mesothelioma is high. (See “Diagnostic workup of atypical mesothelial proliferations.”) If BAP1 is intact with no loss of expression, studies to evaluate for loss of MTAP expression and FISH testing for CDKN2A homozygous deletion should be strongly considered. In a separate study, the authors have demonstrated that the use of BAP1 immunohistochemistry and FISH for CDKN2A deletion in effusion specimens can establish the diagnosis of mesothelioma earlier, even in cases morphologically interpreted as negative. The routine use of BAP1 immunohistochemistry and/or FISH for CDKN2A deletion should be considered only after a rigorous validation process. The use of MTAP immunohistochemistry can be helpful in problematic cases of fluid cytology, especially when the result of BAP1 is equivocal. If MTAP is intact or FISH does not show homozygous deletion, such cases should be designated as “suspicious for malignancy” and surgical tissue sampling should be recommended.
The differential diagnosis of malignant mesothelioma, especially epithelioid mesothelioma, is broad; however, certain morphologic features (such as parakeratotic cells, cell-in-cell engulfment, multinucleation, and large mulberry-like clusters) are helpful clues to considering malignant mesothelioma on cytology. While there is no recommendation on the exact antibody panel (vis-a-vis number and type of antibodies), it is recommended that appropriately validated antibodies with specificity and sensitivity greater than 80 percent be used. The panel should include immunohistochemical stains that confirm mesothelial differentiation (calretinin, WT1, D2-40, and KRT5/6) with the caveat that some of these will occasionally be positive in adenocarcinomas and squamous carcinomas. The panel must be expanded if morphology or clinical history suggests the possibility of metastatic disease. The authors have included a detailed table that describes cytological pitfalls and the immunohistochemical workup of selected epithelioid malignancies in the differential diagnosis of epithelioid mesothelioma. Of note, while PAX8 and GATA3 are excellent markers of renal cell and breast origin, both might be expressed in mesotheliomas.
The article by Louw, et al.,2 explores the boundaries of mesothelioma in situ within pleural effusion samples and any implications for cytologic evaluation. The authors detected abnormalities of BAP1 immunohistochemistry and/or CDKN2A FISH in patients with pleural mesothelioma who in their initial specimen (at least two years prior) did not meet the diagnostic criteria for pleural mesothelioma. Despite the limitations of the study (retrospective design, small cohort, paucity of cells, archived cell blocks), their study highlights the possibility of a cytological diagnosis of early mesothelioma/equivalent for mesothelioma in situ in the correct clinical setting.
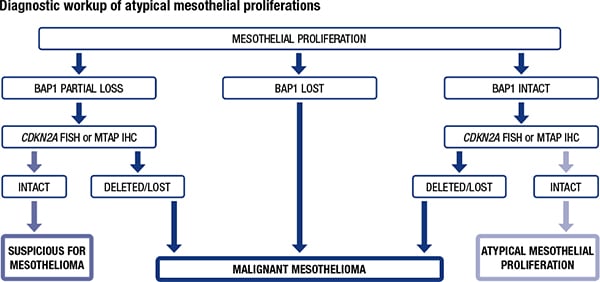
Monaco SE, Brcic L, Dacic S. State-of-the-art cytology of pleural fluid, focusing on the diagnosis of mesothelioma. Cytopath. 2022;33:57–64. https://doi.org/10.1111/cyt.13055. (Adapted from: Beasley MB, et al. Virchows Arch. 2021;478[1]:59–72.)
The last article, by Girolami, et al.,3 is a systematic literature review that evaluates multiple biomarkers for sensitivity and specificity. BAP1 loss by immunohistochemistry carries very high specificity (99 percent) but a sensitivity of only 65 percent; CDKN2A deletion and MTAP loss also each have high specificity but even lower sensitivity. The use of both CDKN2A deletion and BAP1 loss immunohistochemistry provides a higher sensitivity of 83 percent and maximal 100 percent specificity. The importance of internal positive controls is stressed since both BAP1 and MTAP testing depend on the loss of staining in neoplastic cells. In conclusion, this paper also recommends a combined approach using multiple markers and careful validation of methods.
- Monaco SE, Brcic L, Dacic S. State-of-the-art cytology of pleural fluid, focusing on the diagnosis of mesothelioma. Cytopathology. 2022;33(1):57–64.
- Louw A, van Vliet C, Peverall J, et al. Analysis of early pleural fluid samples in patients with mesothelioma: a case series exploration of morphology, BAP1, and CDKN2A status with implications for the concept of mesothelioma in situ in cytology. Cancer Cytopathol. 2022;130(5):352–362.
- Girolami I, Lucenteforte E, Eccher A, et al. Evidence-based diagnostic performance of novel biomarkers for the diagnosis of malignant mesothelioma in effusion cytology. Cancer Cytopathol. 2022;130(2):96–109.
Dr. Manucha is a professor at the University of Mississippi Medical Center, Jackson, and Dr. Davey is a professor of pathology and associate dean for graduate medical education at the University of Central Florida, Orlando. Both are members of the CAP Cytopathology Committee.

