Charna Albert
September 2022—A single high-sensitivity cardiac troponin T measurement below the limit of quantitation of 6 ng/L is a safe and rapid method to identify a substantial number of patients at low risk for acute myocardial injury and infarction, say the authors of a recently published study (Sandoval Y, et al. Circulation. 2022;145[23]:1708–1719).
Allan S. Jaffe, MD, senior author of the study and professor of both cardiology and laboratory medicine and pathology at Mayo Clinic in Rochester, Minn., said Mayo Clinic developed a two-hour algorithm and did not initially embrace the single-sample rule-out. “That’s not because there wasn’t good data about the single-sample rule-out with cardiac troponin T. There actually was,” Dr. Jaffe said in a session at this year’s AACC annual meeting. In fact, he and his coauthors write in the study, extensive data from outside the U.S. support the single-sample rule-out when hs-cTnT concentrations are below the limit of detection of 5 ng/L. However, the FDA does not permit reporting values down to that level. The lowest reportable level is less than 6 ng/L, and Dr. Jaffe notes that the data for using that value are much less robust.

“One of the reasons this works—and this is important and not often talked about—is not just because there is the time that allows for the egress of troponin to get to the circulation, but because if you look at all the risk factors that lead to underlying cardiovascular and atherosclerotic disease, they almost all cause modest increases in troponin values, albeit within the normal range.” So a very low troponin value, he said, not only can exclude myocardial infarction in most instances but also is an indication that the patient doesn’t have a large number of risk factors for atherosclerotic disease.
“The reason we went to a two-hour protocol as well as not using the first sample rule-out has to do with the analytics of the assay,” he said. An imprecision profile from one of the original studies of the Roche high-sensitivity cardiac troponin T assay shows that in distinguishing between a change of 3 ng/L and a change of 5 ng/L, “which is a distinction advocated for use with the one-hour protocol, you’re going to have some misses and some overlaps,” he said, and the same is likely to happen in distinguishing between a value of less than 5 ng/L (limit of detection) and less than or equal to 6 ng/L (limit of quantitation) (Saenger AK, et al. Clin Chim Acta. 2011;412[9–10]:748–754).
This problem related to imprecision is not unique to high-sensitivity cardiac troponin T. Dr. Jaffe and others found that the value of Abbott’s high-sensitivity cardiac troponin I assay can change when repeated on the same sample over a period of time, which calls into question the clinical applicability of the European Society of Cardiology 0/1-hour algorithm to rule out and rule in myocardial infarction. They took 50 random heparin plasma samples (stored at room temperature) and measured for high-sensitivity cardiac troponin I at three times, all within 3.5 hours of the first measurement. Their goal was to evaluate the analytical variation of results in the same samples when measured multiple times over a period and to determine the misclassification rate associated with the European Society of Cardiology 0/1-hour algorithm and the two-hour algorithm due to short-term analytical variation (Kavsak P, et al. Clin Chem. 2017;63[6]:1163–1165).
Almost half (24) of the samples had values that might be applied at the rule-in or rule-out level—either very low (﹤7 ng/L) or within 10 ng/L of the rule-in value (52 ng/L). Seven of the samples would have resulted in a different categorization, depending on the sample reported. This was the case in particular with values that might be used at one hour (2 ng/L versus 6 ng/L), where six of the 18 patients would have switched diagnostic categories from rule-out to observe, Dr. Jaffe said. “So a third of patients would have shifted diagnostic categories just by repeating the same sample, and it’s a reflection of the imprecision of the assays, particularly at lower values.”
In addition, during Mayo Clinic’s analytic validation, substantial differences for hs-cTnT were found among the various instruments (Donato LJ, et al. Am J Clin Pathol. 2021;156[6]:1121–1129). “In addition, we had a flyer rate of 3.4 percent using a change rate of 3 ng/L, and a flyer rate of one percent using a change rate of 10 ng/L,” he said. “These were the reasons why we were concerned that if we used the single-sample rule-out of 6 ng/L, or a delta trying to distinguish in the one-hour algorithm between three and five, we were for sure going to misclassify substantial numbers of patients.”
“That’s why we went to a two-hour protocol and did not embrace single-sample rule-out.”
This was the reality for high-sensitivity cardiac troponin T, but for many assays “using single values substantially above the limit of detection—and therefore reportable—allowed one to rule out substantial numbers of patients.” But for troponin T, the value validated in Europe for single-sample rule-out was less than 5 ng/L, a concentration threshold that isn’t available for clinical use in the U.S. And in Europe, Dr. Jaffe and his coauthors write in Circulation, troponin testing isn’t used as broadly as it is in the U.S., so European data from more selected chest pain populations may not be as informative for U.S. practice. “The FDA only allows reporting for troponin T to a value of less than 6 ng/L, because of the imprecision of values below that number. So one had to ask the question, could a value of less than six be equally good?”
[dropcap]I[/dropcap]n their recent study published in Circulation, the goal of Dr. Jaffe and his coauthors was, first, to determine whether a single high-sensitivity cardiac troponin T (Roche Elecsys Troponin T Gen 5 Stat) below the limit of quantitation of 6 ng/L is a safe strategy to identify patients at low risk for myocardial injury. Second, to evaluate the use of this approach in identifying patients at low risk for acute myocardial infarction, they examined the combined use of a nonischemic ECG with a hs-cTnT of less than 6 ng/L in an adjudicated cohort.
For the first goal, they drew on data from the CV Data Mart Biomarker cohort, a multicenter (22 sites), observational biomarker study involving consecutive adult patients who presented to a Mayo Clinic emergency department and in whom at least one hs-cTnT measurement was obtained within 12 hours of presentation from the date of site-specific hs-cTnT implementation until December 2020. A total of 85,610 patients were evaluated (mean age 63 and 50 percent women). Of the total, 24,646 (29 percent) had a baseline hs-cTnT of less than 6 ng/L. Of these, 49 (0.2 percent) had acute myocardial infarction diagnoses based on ICD-10 codes and 19 (0.1 percent) deaths occurred during the index presentation.
Sex-specific analyses demonstrated that women were more likely than men to have a baseline hs-cTnT of less than 6 ng/L (38 percent versus 20 percent of men, P﹤0.0001). And compared with men with hs-cTnT less than 6 ng/L, women with hs-cTnT less than 6 ng/L were older and more likely to have comorbidities, except for previous myocardial infarction and coronary artery disease, which were more frequent in men.
Acute myocardial injury (any subsequent hs-cTnT increase above the sex-specific 99th percentile) occurred in 146 (1.2 percent) of the 11,962 patients with a baseline hs-cTnT of less than 6 ng/L with serial measurements, resulting in a negative predictive value of 98.8 percent (95 percent CI, 98.6–99.0) and sensitivity of 99.6 percent (95 percent CI, 99.5–99.6). Among the patients who developed acute myocardial injury, maximum hs-cTnT concentrations were 20 (14–43) ng/L.
“The negative predictive value of less than six for men was very high,” Dr. Jaffe said. “For women, on the other hand, there was an occasional signal that suggested it was less than perfect, particularly in older women, usually with cardiovascular comorbidities.” Of the 146 false-negative cases, 117 were women and 29 were men. Among those with a baseline hs-cTnT of less than 6 ng/L, 0.7 percent of men (29/4,264) and 1.5 percent of women (117/7,698) developed acute myocardial injury. Adjudication of the 146 cases demonstrated that 76 percent (111) were attributable to isolated nonischemic acute myocardial injury. The remaining 35 cases (25 women and 10 men) were classified as acute myocardial infarction.
In a separate adjudicated cohort, a nonischemic ECG with hs-cTnT of less than 6 ng/L identified 33 percent of patients (610/1,849) as low risk and resulted in a negative predictive value and sensitivity of 100 percent and a 30-day rate of 0.2 percent for myocardial infarction or death.
Among the 624 patients with a baseline hs-cTnT of less than 6 ng/L, 206 (33 percent) had serial hs-cTnT measurements. In those with a two-hour serial measurement, concentrations remained less than 6 ng/L in 84 percent of patients (173/206). Within 24 hours of the initial baseline of less than 6 ng/L, two patients (0.97 percent) developed acute myocardial injury. Among patients with a baseline hs-cTnT of less than 6 ng/L, there were no differences in myocardial infarction or death between those with a two-hour hs-cTnT that remained less than 6 ng/L in comparison with those with a two-hour hs-cTnT of greater than 6 ng/L but below the sex-specific 99th percentile.
“What you can see first of all is that when you do serial sampling, the frequency when you’re less than six of staying less than six is extremely high, and very few people had values above it,” Dr. Jaffe said. “More importantly, when you have values of less than the limit of quantitation—which is what six is, from the FDA perspective—you still have a very robust negative predictive value. In the adjudicated subset it was 100 percent if one had a normal electrocardiogram.”
“So the single sample rule-out isn’t perfect,” he continued, referring to the slight signal in older women, “but it’s worth using.” And earlier data showed that if the test is done too early after symptom onset—that is, in less than two hours—“one ends up having less than the magic 99 percent negative predictive value,” he said. That 99 percent negative predictive value comes from a study in which emergency medicine physicians were asked what percentage of misses they could tolerate, “and it was one percent at 30 days.” So these patients have to be at least two hours from the onset of symptoms, he said, and according to the European Society of Cardiology guidelines, three hours from symptom onset. “And then with every high-sensitivity assay, recognizing the need for unique cutoff values for each assay now including troponin T, the single-sample rule-out can be used.”
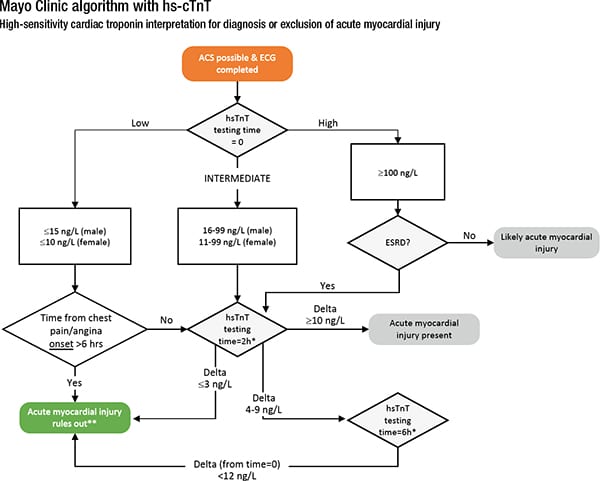
Dr. Jaffe shared the two-hour algorithm generated at Mayo Clinic in Rochester, without the single-sample rule-out (see “Mayo Clinic algorithm with hs-cTnT”).
A Mayo Clinic study published last year evaluated the impact of transitioning from the contemporary fourth-generation Roche cTnT assay to the Elecsys Troponin T Gen 5 Stat assay on the incidence of myocardial injury and infarction diagnoses and on resource use (Ola O, et al. J Am Coll Cardiol. 2021;77[25]:3160–3170). “There is a modest increase in MIs, particularly in type two MIs, and it’s in both men and women,” Dr. Jaffe said, “although the magnitude is a little greater in women.” But the biggest change, he said, is the change in myocardial injury—from 11 percent to 38 percent.
“So this is the challenge that clinicians worry about all the time,” he said. “‘How do I know if this weak and dizzy person fits as myocardial injury or a subtle MI when the ED has gotten troponins on all of them?’” If laboratories educate—and the laboratorians and clinicians spent six months at Mayo educating pre-transition—“the protocol seems relatively effective,” Dr. Jaffe said. And despite the marked increase in myocardial injury and modest increase in MI, overall resource use didn’t increase, except for angiography. “Among those without cTnT increases,” the authors write, “there were more ED discharges and fewer cardiac tests.”
[dropcap]I[/dropcap]n his AACC session, Dr. Jaffe presented the case of a 78-year-old woman with a history of hypertension and chest pain for two years with a negative workup looking mostly for arrhythmias. Her chest pain increased in the prior six months and could last up to two days, and before arriving at the emergency department she’d had a day’s worth of tightness. “She had had a stress test a couple years before so the ED did a CT pulmonary embolism study, which was normal,” he said, so she was admitted to ischemic heart service.
Her two hs-cTnT values were 10 ng/L. Dr. Jaffe was going to see her and ask for a third value because he was concerned she might be a so-called late presenter on the downslope of the troponin time-concentration curve. “But she was off getting an echo. They called back to say she had a regional wall motion abnormality in her septum. She had a negative angiogram and no coronary disease, but she had a profusion defect by MRI in her septum.”
“This is a good example of what’s called MINOCA—myocardial infarction with nonobstructive coronary arteries,” he continued. “There are a variety of flavors of this, from spasm to microvascular disease.” It occurs in up to 10 percent of myocardial infarctions in women, he said, and about three percent in men.
He shared Mayo Clinic’s yield of MRI in patients with elevated cTnT and normal coronary angiograms. “These were patients who came in and were thought clinically to have had ischemic heart disease. However, after they had an angiogram it was thought that they could not have ischemic heart disease, because the angiogram did not manifest obstructive coronary artery disease.” These patients, he said, are ones who might well have MINOCA. They then went for a cardiac MRI. Of 60,421 patients who were admitted with elevated troponins from 2000 to 2016, 18,490 underwent an angiogram within 30 days of admission. A subset (215) of those whose angiograms were negative underwent cardiac MRI. “Of the patients who go for an MRI,” Dr. Jaffe said, “the most common mimicker of MI is myocarditis” (32 percent). “But the second are small infarctions” (22 percent). Twenty percent had nonischemic cardiomyopathy, nine percent had stress cardiomyopathy, and 17 percent were normal (Bhatia S, et al. Heart. 2019;105[16]:1231–1236).
The earlier an MRI is done the better the yield, he said. “I’m not telling you that everyone who has a negative angiogram should get an MRI—that would break the bank. But in selected patients like this, who have a suggestive history or who have regional wall motion abnormalities, it’s reasonable.”
Dr. Jaffe also presented the case of a 68-year-old man with multiple risk factors—hypertension, hyperlipidemia, hyperglycemia, a positive family history of premature coronary artery disease in multiple relatives, and a prior positive coronary artery scan in the past. “Usually he walks three to four miles a day and had been doing so,” but for three days pre-presentation, “he had substernal chest pain radiating to his scapula during his walk,” he said. On the day of admission he had a two-hour episode, and when it recurred he went to the emergency department where it resolved. His electrocardiogram was unremarkable.
High-sensitivity cTnT was 13 ng/L. Two hours later it was 12 ng/L. “So he ruled out for MI,” Dr. Jaffe said. “My colleague, who was working in the ED, said, ‘If this patient really has something, could his troponins stay that low? Am I missing something? Should I do something else?’” Dr. Jaffe’s advice: If the colleague is suspicious, he should. So he did a stress test during which the patient developed his typical pain and marked ST segment elevation indicative of severe ischemia. Subsequently, an angiogram confirmed a severe right coronary artery blockade.
“Now, there’s an important caveat with all this,” Dr. Jaffe said. “First of all, this is a good case of unstable angina. His pain was duplicated during the stress test, and we have an angiogram that was done right away.” But in general, he said, “I would argue there is little unstable angina left.” Many patients who have chest pain, however, will be diagnosed with coronary artery disease as computed tomography angiography becomes more widely used and detects coronary artery disease. “That does not mean they have unstable angina,” he said. “It could just be incidental coronary artery disease. So there’s an important issue to sort that we do not have good criteria for, as to what one ought to do with these sorts of patients.” Though it’s clear that the occasional patient, such as in the case, will have unstable angina, “if we’re not careful, our EDs could be overwhelmed with people who have ruled out but who have CTA imaging and have incidental coronary artery disease.” And that, he said, is going to be a new challenge, given that the 2021 ACC/AHA joint guidelines for chest pain rely heavily on imaging and in particular on CT coronary angiogram.
Charna Albert is CAP TODAY associate contributing editor.

